In-Workflow Tools Are Changing the Conversation and Driving Adherence
By: ConnectiveRx Awareness & Adherence team
For patients struggling with a serious medical condition, finally finding an effective treatment and the ability to get on and stay on that medication can be life-changing. The concept of shared decision-making is important and asking patients what matters to them is a critical part of the process, including the question: “Does the cost of the medication that I would like to prescribe matter to you?” Imagine if healthcare providers (HCPs) could begin the process of prescribing a medication for their patients, and on their electronic health records (EHR) screen is cost information for available products in that category. That scenario is happening now, and it’s called Real-Time Benefit Check.
One of the goals of physicians is to encourage adherence, and they are fully aware that drug costs remain a top reason why patients don’t take their medication as prescribed. With price comparison information within prescribers’ existing EHR systems, they have the ability to discuss with their patients not just which medications are likely to be effective, but also explore the actual out-of-pocket cost of each option at the time of the office visit. This real-time conversation with the patient during the prescribing process facilitates shared decision-making and can also save the HCP time in the long run by preventing rework later in the prescribing process.
The Impact of Real-Time Comparison Drug Pricing on Your Brand
When providers discuss the amount the patient will pay for a prescribed medication while the patient is still in their office, it reduces the likelihood that the patient will leave the pharmacy empty handed and frustrated. While this represents a major step forward, it doesn’t automatically include manufacturer patient savings offers. The potential impact on the provider-patient conversation driven by the inclusion of patient-specific drug prices in the EHR is game-changing.
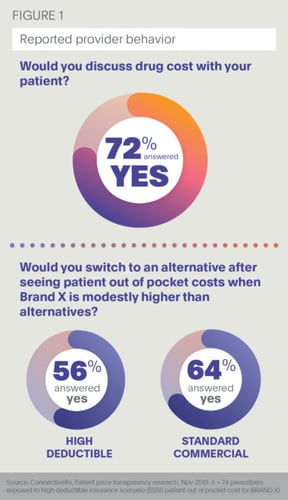
In a ConnectiveRx study of 144 prescribers of oral anti-diabetic medications, 72% report that they would have a discussion about the price the patient will pay for a selected medication, as well as possible alternative therapies, once they view actual out-of-pocket costs (Figure 1). It is creating a new kind of conversation between prescriber and patient.
 HCPs Will Compromise to Help Patient Adherence
HCPs Will Compromise to Help Patient Adherence
Even if a particular brand is the first choice, providers are willing to compromise with patients and select another brand after seeing real-time costs within the EHR. In fact, 56% of prescribers report they would switch to an alternative medication when viewing high-deductible out-of-pocket costs. This number increases to 64% for those patients with standard insurance plans.
Prescribers certainly want to encourage patients to accept their first-choice brands, and 83% of the prescribers surveyed report sharing the reasons they recommend a specific brand. But this doesn’t change the fact that many patients may be either unwilling or unable to accept this medication due to cost. The majority of prescribers (62%) say they will share the reasons that they prefer the first-choice brand but then let the patient decide. Only 21% of providers report they will encourage patients to accept the first-choice brand, with the remaining 17% just focusing the conversation on less expensive choices or some other option.
Looking Beyond Real-Time Benefit Check for True Patient Cost
Importantly, the research also revealed that prescribers only consider the initial pricing information in real-time benefit check, with more than half (57%) reporting they do not factor in that the patient’s cost will go down once their deductible is met. Furthermore, 31% of prescribers assumed patient costs would stay the same, and 26% made no assumptions about future costs.
Based on this data, it is reasonable to assume that conversations about this information are not happening between patients and providers. Providers simply have not had visibility to this additional cost information and can’t discuss with the patient this key financial information to help them make a fully informed decision.
Enter the Non-Commercial Pharmacy
In the case of specialty medications, once a prescriber and patient have agreed on the best and economically informed course of treatment, the next solution in the drive to increase adherence is the non-commercial pharmacy (NCP). Commonly known as distribution channels for product offers, non-commercial pharmacies have the power to streamline the medication enrollment process, eliminating inefficient, time-consuming paper-based processes to reduce the burden on providers, get patients on their therapy faster, and reduce the risk of non-adherence.
NCPs serve as a virtual holding area for a prescription that is sent to a dispensing pharmacy once benefit verifications, prior authorizations (PAs), copay programs, and other fulfillment needs are completed. Prescribers can select a specific NCP at the point of prescribing while remaining in their existing workflow. Rather than spending increased time bouncing between a myriad of portals, the prescription process takes seconds and patients are simultaneously automatically enrolled in a patient support hub.
In addition, instead of exiting the patient’s EHR record and manually filling out a patient enrollment form, the provider selects the non-commercial pharmacy to receive the prescription for the drug, just like they would a retail pharmacy at the point of prescribing. Patient data is already in the EHR, and the relevant information is automatically transferred to the prescription. Patients gain access to their medication days or even weeks faster, and the process gets started with minimal HCP activity, leaving more time for patient interactions.
Make Cost and Savings Offers Visible with ConnectiveRx
Other in-workflow tools provide prescribers and patients with patient education, printable coupons, and financial savings offers that may also help to increase medication adherence. These new tools, embedded within the EHR, are offering providers better clarity, making it easy to view out-of-pocket patient costs and potential savings.
Most importantly, enabling real-time conversation about cost and shared decision-making between providers and their patients helps alleviate patient frustrations and ultimately drives better adherence, a true win for HCP-patient engagement and education. Connect with one of our experts today to learn more.
The Battle of Accumulators and Maximizers: What You Need to Know For 2024
If you missed this insightful discussion - don't worry. Register now and get access to the on-demand recording. Our expert panel gave an update on the current state of the market, the recent copay accumulator court ruling, and more!

